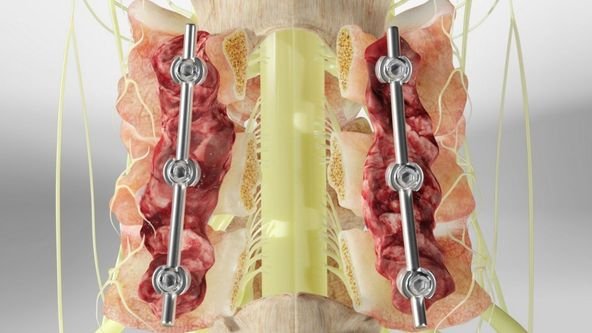
What Is Posterior Cervical Spine Surgery?
Posterior Cervical Spine Surgery is performed from the back (posterior) side of the neck. The main goal is to decompress the spinal cord or nerves, stabilize the spine, and restore proper alignment. It can be performed using different surgical techniques based on the patient’s condition, including:
Laminectomy
Laminoplasty
Foraminotomy
Posterior Cervical Fusion
Minimally Invasive Posterior Cervical Decompression
By creating space around the spinal cord and nerve roots, the procedure reduces pressure, alleviates pain, improves mobility, and prevents progressive neurological damage.
Conditions Treated with Posterior Cervical Spine Surgery
Dr. Ankit Daware recommends posterior cervical surgery for a range of cervical spine disorders where non-surgical treatments do not provide relief. These include:
1. Cervical Spinal Stenosis
A narrowing of the spinal canal that compresses the spinal cord. This may cause numbness, weakness, difficulty walking, and balance problems.
2. Herniated Cervical Disc
A bulging or ruptured disc that puts pressure on the nerve roots, causing neck pain radiating into the arms.
3. Cervical Myelopathy
A serious condition caused by compression of the spinal cord, leading to clumsy hands, gait imbalance, and loss of bladder control.
4. Degenerative Disc Disease
Age-related wear and tear that reduces disc height and causes instability or nerve compression.
5. Cervical Fractures or Trauma
Accidents or injuries that damage spinal structures and require stabilization.
6. Spinal Tumors
Tumors pressing against the spinal cord or nerve roots are often removed surgically from the posterior side.
7. Kyphotic Deformity
Abnormal curvature of the cervical spine requiring correction and stabilization.
Symptoms That May Require Posterior Cervical Surgery
Patients may experience a combination of symptoms, including:
Chronic neck pain
Shoulder or arm pain
Numbness or tingling in hands
Muscle weakness
Difficulty walking
Loss of hand coordination
Reduced grip strength
Headaches
Loss of balance
Shooting pain down the arms
Worsening neurological symptoms
If these symptoms persist despite medications, physiotherapy, or lifestyle modification, Dr. Ankit Daware may recommend surgery to prevent further damage.
Diagnosis and Assessment Before Surgery
Before recommending Posterior Cervical Spine Surgery, Dr. Ankit Daware conducts a thorough evaluation including:
1. Medical History & Physical Examination
Understanding pain pattern, mobility restrictions, and neurological symptoms.
2. Imaging Tests
X-ray to check alignment
MRI to assess nerve compression
CT scan to evaluate bone structure
EMG/NCV studies if nerve damage is suspected
3. Non-Surgical Treatment Review
Ensuring physiotherapy, medications, or injections were tried before surgery becomes necessary.
4. Risk Assessment & Planning
A customized surgical plan is made based on the patient’s age, spinal condition, lifestyle, and overall health.
Types of Posterior Cervical Spine Surgeries
Dr. Ankit Daware performs a variety of posterior cervical procedures. The most common types are explained below:
1. Posterior Cervical Laminectomy
A laminectomy removes the lamina (back portion of a vertebra) to create space for the spinal cord. It is useful for patients with:
Cervical myelopathy
Multi-level stenosis
Spinal cord compression
Laminectomy offers immediate relief by decompressing the spinal structures.
2. Posterior Cervical Laminoplasty
Laminoplasty involves reshaping and opening the lamina like a “door” to enlarge the spinal canal. It preserves more bone compared to laminectomy and maintains spinal stability.
Ideal for patients with:
Multi-level compression
Myelopathy
Chronic stenosis
3. Foraminotomy
A minimally invasive procedure where the foramen (nerve root exit passage) is enlarged to relieve nerve pressure.
Recommended for:
Arm pain
Pinched nerve
Foraminal stenosis
4. Posterior Cervical Fusion
Fusion stabilizes the spine using bone grafts and metal implants such as rods and screws. It is performed when instability is present.
Useful for:
Trauma
Severe degenerative changes
Tumors
After laminectomy for stability
5. Minimally Invasive Posterior Cervical Surgery
Dr. Ankit Daware specializes in minimally invasive techniques that:
Reduce blood loss
Minimize muscle damage
Enable quicker recovery
Require smaller incisions
These advanced procedures lead to faster healing and a faster return to daily activities.
How Posterior Cervical Spine Surgery Is Performed
Although each surgery type differs, here is the general step-by-step process:
Step 1: Anesthesia
General anesthesia ensures the patient is completely asleep and pain-free during the surgery.
Step 2: Positioning
The patient lies face down. The neck is positioned carefully to ensure safety and access.
Step 3: Incision
A small incision is made in the midline of the back of the neck.
Step 4: Exposure
Muscles are gently separated to reach the cervical vertebrae.
Step 5: Decompression or Fusion
Depending on the procedure:
Lamina is removed or reshaped
Nerve root pathways are enlarged
Tumor is removed
Rods and screws are placed for fusion
Step 6: Closure
Layers of tissues are carefully closed, and a dressing is applied.
The surgery typically lasts between 1 and 3 hours depending on the complexity.
Benefits of Posterior Cervical Spine Surgery
Patients treated by Dr. Ankit Daware often experience remarkable improvements such as:
Relief from neck and arm pain
Restoration of mobility
Improved hand coordination
Better balance and gait
Reduced numbness and tingling
Prevention of further spinal cord damage
Improved quality of life
In cases of severe myelopathy, surgery stops the progression of neurological deterioration, which is crucial.
Recovery After Posterior Cervical Spine Surgery
Recovery varies by patient, but most individuals notice significant improvement within weeks. Key recovery details include:
Hospital Stay
Usually 2–4 days depending on the procedure.
Pain Management
Pain medications and muscle relaxants reduce discomfort.
Neck Collar
Some patients may need a cervical collar for support during healing.
Movement & Activity
Walking is encouraged early
Heavy lifting is avoided
Driving is postponed until medically cleared
Physiotherapy
Strengthening exercises restore mobility and neck stability.
Return to Work
Office jobs: 2–4 weeks
Manual labor: 6–12 weeks
Dr. Ankit Daware provides personalized recovery plans based on surgery type and patient health.
Frequently Asked Questions (FAQ)
1. Is Posterior Cervical Spine Surgery painful?
Some postoperative soreness is normal, but pain is well controlled with medications.
2. How long does recovery take?
Most patients recover within 4–8 weeks. Those undergoing fusion may take longer.
3. Will I need physiotherapy?
Yes, physiotherapy is essential for strengthening and regaining mobility.
4. Is surgery the only option?
No. Surgery is recommended only when non-surgical treatments fail.
5. When can I resume normal activities?
Light activities within days, moderate work in a few weeks, and strenuous work after complete healing.
